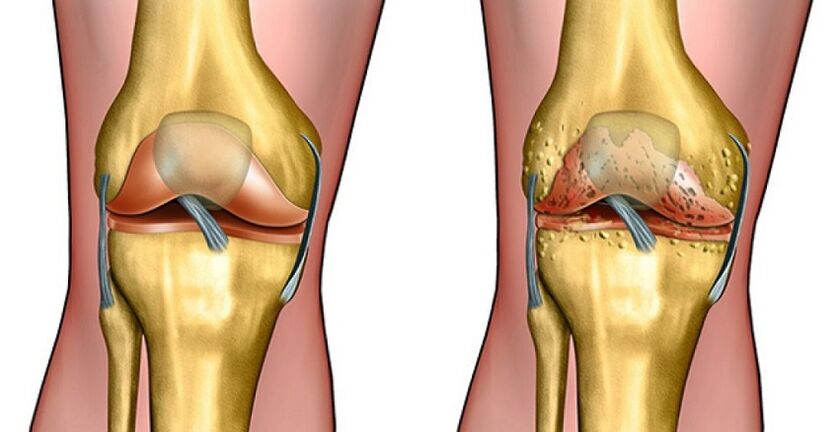
Today, the disease of osteoarthritis of the joints has become the most common among all pathologies of the musculoskeletal system. In addition, city dwellers, people used to leading a sedentary lifestyle and those who have recently suffered injuries of varying intensity, most often suffer from joint disorders.
Doctors' forecasts in this regard are disappointing. It is assumed that in the near future, the number of people suffering from various forms of osteoarthritis of the large joints will only increase. According to the latest data, about 7% have experienced all of the symptoms and consequences of osteoarthritis.
This disease has become one of the main causes of disability and reduced performance. Characteristically, the maximum incidence occurs in the 40-60 year age groups, and not just in older retirees, as is mistakenly believed.
What is osteoarthritis?
Osteoarthritis (another name for osteoarthritis) should be understood as a complex degenerative disease in which the cartilage plate of the bone that forms the joint is destroyed. The reasons do not lie only in the processes occurring in the hyaline cartilage.
There are many other prerequisites for the disease.
Osteoarthritis of the joints develops under the condition:
- excessive physical activity. Usually overweight people get sick in such cases. Human joints are not designed for constant movement with a heavy load. For this reason, the increased compression experienced by the knees during activity becomes a prerequisite for micro-trauma of cartilage tissue. There is a violation of the sliding properties of tissues and a decrease in joint mobility. Athletes often suffer who have systematically damaged joints due to sudden and frequent changes in natural pressure between the surfaces of the joint or a high load with insufficiently heated joints;
- congenital or acquired malformations, lesions of the musculoskeletal system. Under such conditions, the disease is caused by improper contact of the articular surfaces of the bone. Absolutely, the whole load can not be distributed over the joint, and injuries are formed in places of excessive compression. A vivid example of such a violation will be rickets, scoliosis and kyphosis. It should also include incorrect fusion of broken bones, various deformities of the limbs;
- violation of the regeneration of cartilage. This mechanism of the development of osteoarthritis is observed in the presence of an inflammatory process in the body, impaired blood circulation and hormonal disturbances. The problem is based on an inadequate restoration of the lost cartilage tissue, a lack of natural remodeling and thinning;
- problems with the formation and production of synovial fluid. With insufficient joint fluid, the friction surfaces are constantly injured, their wear and inflammation accelerate, the general condition of the body worsens.
Stages of osteoarthritis
Since osteoarthritis of the disease provokes the destruction of the cartilage tissue of the joint, its symptoms vary greatly depending on the stage of the pathological process.
As a result of the active destruction of the joint surface, a person will experience new symptoms, and the prognosis for the restoration of motor activity will not change. Based on the clinical picture of the disease, the doctor will choose the optimal method of treatment and drugs.
Osteoarthritis of the 1st degree is characterized by the fact that discomfort and slight pain are felt only after prolonged intense exertion. After a short rest, the signs that appeared during physical activity fade.
In this case, the joint damage will not be visible on the X-ray photo, but a slight narrowing of the joint space is possible.
Stage 2 of the pathology is characterized by an increase in symptoms. Now there is pain not only from prolonged activity, but also from minor movements of the limbs.
Rest will not provide the desired relief. There is stiffness in the movements, the mobility of the joint is limited. It is recommended at this stage to reduce the load on the affected joints, but this should not be completely ruled out, otherwise muscle atrophy occurs. An x-ray will show clear signs of osteoarthritis:
- bone growth;
- deformation;
- neoplasms (osteophytes) near the joint space, its narrowing.
When the disease reaches its final stage, lesions in the joints cause constant excruciating pain. Therefore, at the reflex level, a person begins to strongly restrict his movements, to protect the affected joint from stress. Pain syndrome occurs even during sleep and rest, when the joints are at rest.
The patient is forced to take the position in which it hurts the least. Movement is only possible with the help of a wheelchair or crutches.
It is characteristic that the 3rd and 4th degree of osteoarthritis can completely deprive a person of the ability to walk due to the fusion of joint surfaces (ankylosis).
Which joint is most often affected?
According to medical statistics, the lower limbs are the most susceptible to osteoarthritis. The joints suffer from inflammation and degeneration: hip, knee.
With hip joint problems, pelvic pain is initially felt after a long walk or run. With the active progression of the pathology, the pain intensifies and mobility is limited.
A person will notice unpleasant stiffness in the joint, and in some positions the stiffness increases several times at a time. In the later stages of osteoarthritis of the hip joint, the patient unconsciously protects the affected leg and tries not to step on it at all. He doesn't move his pelvis, which helps relieve the pain.
Osteoarthritis of the knee joint is manifested by discomfort and aching pain after walking. There are no external manifestations of the problem and inflammation. The most common prerequisite for osteoarthritis of the knee joint is its past trauma against the background of damage to internal structures.
Such lesions, as a rule, cause abnormalities in the contiguity of the joint surfaces in contact. Also takes place:
- overloading of certain areas of the cartilage;
- their rapid wear.
The changes, as in the previous case, depend on the degree of osteoarthritis. You should also take into account the causes of the disease, the availability of adequate medical care, the general condition of the body and the dynamics of the pathological process. Some forms of the disease do not make themselves felt for a long time and do not progress.
Sometimes, even for decades, there is no obvious deterioration of the knee. In other cases, there is a rapid increase in symptoms and a high probability of loss of mobility.
Get rid of osteoarthritis
Today there are 2 main directions in the treatment of osteoarthritis of large joints: medical and surgical.
First of all, the treatment is aimed at rapidly improving blood circulation in the diseased joint and accelerating the properties of cartilage tissue with the help of drugs. Anesthesia and elimination of inflammation are also necessary. For these purposes, doctors practice the use of the following drugs.
Nonsteroidal anti-inflammatory drugs (NSAIDs)
These drugs interfere with the natural chemical chain in cartilage which causes inflammation. There is swelling of the tissues, pain appears, and the strength of the cartilage decreases during movement.
Through the use of anti-inflammatory drugs, it is possible to reduce or completely stop the pain syndrome. The initiation of the so-called chain inflammatory process is also prevented, which helps to accelerate the regeneration of the affected areas.
Medicines are produced in the form of tablets, powder and rectal suppositories. The tactics of treatment, the choice of a specific drug is determined by the doctor strictly on an individual basis, depending on the clinical picture of the disease, its dynamics and concomitant pathologies.
Opioids and chondroprotectors
Strong, centrally acting pain relievers are called opioids. Usually, these drugs have a narcotic effect on the body, increasing the thresholds of pain sensitivity. Through this treatment, the pain in the affected joints can be reduced.
The use of drugs in this group should be strictly under the supervision of the attending physician, since these drugs lead to mental and physical dependence.
To accelerate the restoration of cartilage tissue, special means are used - chondroprotectors. They are, on the whole, the structural elements of the cartilage itself, which allows them to have an activating effect on their recovery.
These drugs include:
- chondroitin sulfate;
- glucosamine sulfate;
- hyaluronic acid.
Chondroitin and glucosamine are organic substances abundant in the intercellular space of the cartilage. The mechanism of their action on the joints has not yet been fully understood, however, it has been repeatedly proven to have a positive effect on the regeneration of cartilage tissue during treatment.
Chondroitin drugs activate the production of special substances from the extracellular matrix of cartilage (proteoglycans and hyaluronic acid). At the same time, the process of resorption in the tissues is significantly inhibited. In the same way, some chemical processes are suppressed, there is a decrease in the inflammation of the cartilage, damage and the severity of the pain syndrome.
Long-term use of drugs in this group is often necessary. A course of treatment is required for at least 6 months. Otherwise, the benefits of the therapy should not be expected. The organic combination of chondroitin and glucosamine is more commonly practiced. However, clinical studies have not confirmed a significant difference between such treatment and the use of just one of the chondroprotectors.
Despite the obvious benefits and safety, not everyone can treat osteoarthritis of the joints with such drugs due to the relatively high cost.
Hyaluronic acid is no less common in modern medicine. It is a long chain of carbohydrates that gives elasticity and viscosity to the synovial fluid. The unique properties of hyaluron are largely responsible for the good sliding properties of joint fluid.
Intra-articular injections of the drug have a good effect on the condition of the body, as studies have shown that osteoarthritis is often triggered by a decrease in the concentration of hyaluron inside the joint and a shorteningof the chain of its molecules.



















