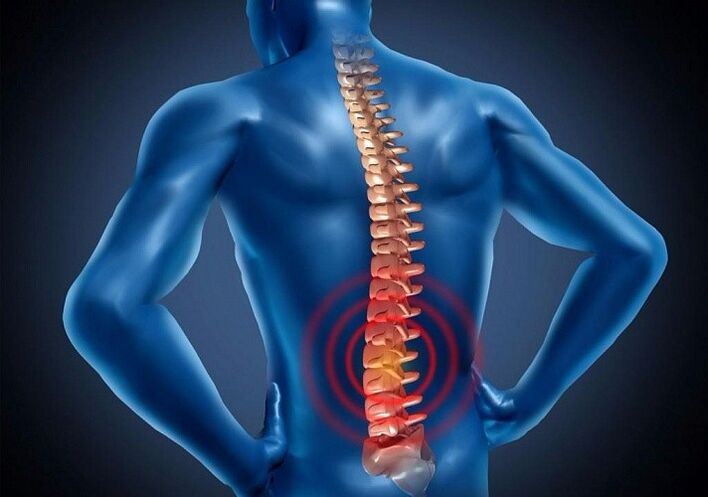
Lumbar osteochondrosis is a dangerous disease of the spine, characteristic of people who have reached the age of 35 and older. The natural wear and tear of the joints provokes the development of pathology. Untimely access to a rheumatologist, in most cases, leads to disability. Modern medicine offers many effective methods of treatment in the primary stages. Early diagnosis is the key to a healthy life without restrictions.
Lumbar osteochondrosis - general definition
Osteochondrosis of the lumbar spine is a process of dystrophic degeneration in the intervertebral cartilaginous formations - discs.
Discs provide the main functions of the spine - the ability to move and bend, resistance to stress. As a result of pathology, important elements become thinner, deformed, vertebrae are aligned, nerve endings and blood vessels are pinched. Negative processes are accompanied by painful sensations of varying intensity and limitation of motor function.
Pathology causes changes in the connecting elements of the spine - cartilage, bones, discs and joints. It is caused both by natural wear processes and by acquired diseases of the joints or the result of an improper lifestyle.
causes
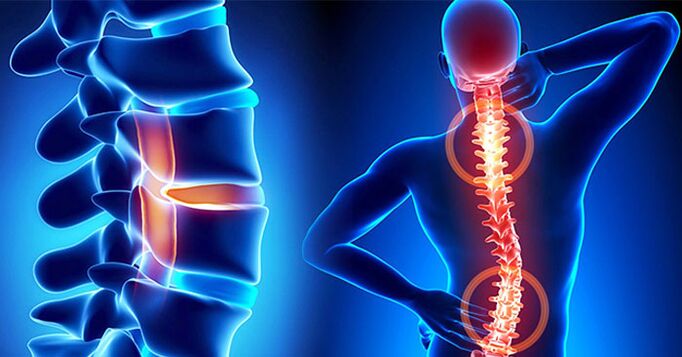
There can be several reasons for the development of lumbar osteochondrosis:
- Natural or premature wear of the body;
- Excessive load on the lower back - lifting loads, working "on your feet" or a sedentary, "sedentary" lifestyle;
- Genetic predisposition to joint diseases, such as rheumatoid arthritis;
- Violation of metabolism, leading to the accumulation of toxic substances in the connecting discs;
- Chronic diseases of the circulatory system. Nutrients and trace elements cease to penetrate into the cartilage tissue in the proper amount. Hypoxia sets in, which contributes to the destruction of the intervertebral joints;
- Autoimmune pathologies.
Secondary factors can also provoke the development of lumbar osteochondrosis:
- Chronic injuries, back bruises;
- Exceed the weight norm by more than 15-20%;
- Heavy or power sports;
- Constantly wearing uncomfortable shoes. High heels, tight shoes, rubber or sports shoes are the first enemies of the spine;
- Valgus changes in the foot;
- Scoliosis, kyphosis, diabetes mellitus, spinal tuberculosis;
- Impact of low temperatures.
clinical picture
Symptoms of lumbar osteochondrosis depend entirely on which nerve roots are affected by the disease. The degree of compression of the vertebrae, the stage of the disease and the damage to the disc determine the signs.
Rheumatologists distinguish the following main symptoms:
- Violation of tactile susceptibility in the lumbar region. Numbness extends to inner thighs and groin. Can affect one or both limbs;
- There is a sharp, stabbing pain in the lower back. The big toe completely loses its mobility and a characteristic numbness is observed;
- Loss of normal foot function, tenderness in fingers, lower leg and outer thigh. In these parts of the leg there is a tone and regular convulsive attacks. On examination, there is no Achilles reflex;
- If the disease affects the lower root artery, then there is complete paralysis of the muscles of the buttocks, the back of the thighs and the perineum. There is a severe violation of motor function, up to complete immobility.
With lumbar osteochondrosis, not only the nerve endings of the spine are affected, but also the blood vessels.
The following specific signs depend on the type of lesion:
- When only the nerve roots are disturbed, a change in the patient's gait is observed. The pain is localized not only in the lumbar area, but also in all parts of the legs. Radicular syndrome is characterized by constant pain. Usually one-sided. In the lower back, there are tingling and aches. The pain can be relieved with some exercise.
- Compression of blood vessels causes perfusion in the hip area. As a result, oxygen starvation of spinal discs occurs. Painful sensations arise when walking in the buttocks, thighs and lower back. Completely removed after a night's rest.
Simultaneous violation of the functionality of blood vessels and nerve roots can lead to irreversible deformation of the discs. Spine-like bony growths form in the movable joints of the lower back. This leads to severe pain and makes normal natural movement impossible. Violated posture, gait. As it progresses, complete paralysis may occur.
Disease stages
Lumbar osteochondrosis develops gradually, in several stages. Each stage has its own characteristics, which determine the degree of progression.
- I stage.The slow destruction of the intervertebral discs begins. The process can last from several months to 2 to 5 years. Manifested by minor pain, discomfort in the inguinal and femoral muscles. It is noticed when walking or when the weather changes.
- II stage.The collagen fibers of the fibrous rings of the spine are drawn into the negative process. The space between individual vertebrae is rapidly shrinking. Rubbing appears, which causes strong attacks of pain. Violated gait, posture, arch appears. Lumbar osteochondrosis is most often diagnosed at the second stage of the course.
- Stage III.An intervertebral hernia appears. And if the patient did not have to consult a doctor for the symptoms of stage II, it will no longer be possible to ignore the excruciating pain of the third stage. The deformation of the bones and joints of the spine in the lumbar area is already irreversible. Walking takes a lot of effort. This is due to the pain and the impossibility of relieving it with conventional painkillers.
- stage IV.Partial or complete impairment of motor function. At this point, the patient is assigned a disability group. Threaten complete paralysis. Vital activity is impossible without taking a wide range of drugs.
Diagnostic measures
Diagnostic measures include several techniques and begin with collecting a complete history of the disease. During the initial consultation with a rheumatologist, the following data is clarified:
- The patient's complaints are carefully analyzed - the place of localization of pain, where discomfort is still felt, in which parts of the hip joint there is a feeling of heaviness, convulsions, etc. ;
- Duration, regularity, nature of the pain;
- When the first symptoms, even minor ones, appeared. How long has passed since the last attack, what causes the discomfort and what factors contribute to its elimination;
- Surrounding living conditions of the patient. Profession, work, household load, sports and the presence of additional factors for increased physical activity (dacha, garden, hobbies associated with weight shifting);
- Review of the history of illnesses the patient has suffered from in the past or present.
After collecting the clinical picture, the rheumatologist proceeds directly to the external examination. During the examination, the gait, the anatomical position of the legs, arms, torso, in relation to the spine are analyzed. The skin is examined for changes - pigmentation, peeling, eczema, rashes, etc. An assessment of motor function is given.
Performing simple exercises - tilting forward, backward, raising arms and legs, turning the head, rotating movements of the pelvis, the patient allows the doctor to determine the degree of damage to the spinein the lumbar region.
The final measures of the external examination are actions to determine the degree of root involvement:
- Symptom Lasegue.Lying on his back, the patient alternately raises his legs, bent at the knee. If it causes pain in the lower back, the readings are considered positive.
- Dejerine Symptom.The patient is asked to tighten the abdominal muscles as much as possible. The occurrence of discomfort in the spine indicates the development of lumbar osteochondrosis.
- Neri Symptom. Strong forward and backward tilts of the head respond with pain in the lower back.
- Wasserman symptom. The patient, in the supine position, moves the leg to the side as much as possible. In the presence of pathology, unpleasant pain occurs in the groin and front of the thigh.
To confirm or exclude the diagnosis, the patient is invited to undergo instrumental diagnostics. MRI is considered the most effective way to determine lumbar osteochondrosis. The study shows the distance between the vertebrae, the development of neoplasms and bone deformities. It may be contraindicated in patients with mental disorders.
Computed tomography gives a fairly accurate picture of the disease in one plane - horizontal or vertical.
X-rays are used only in the final stages, when irreversible changes in the bone tissue of the spine begin.
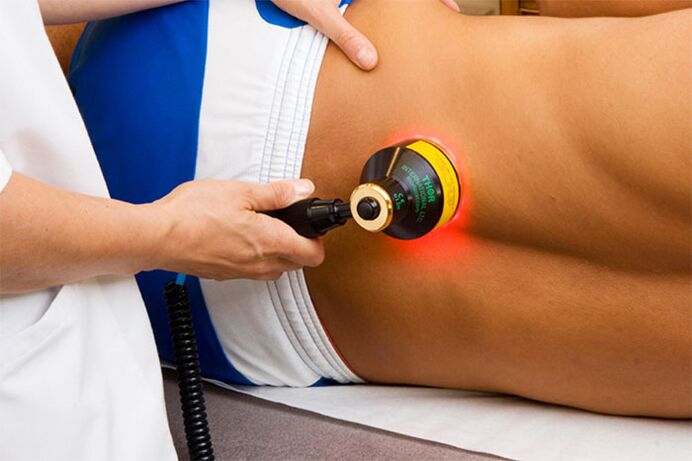
Complex treatment of lumbar osteochondrosis
The causes of the pathology have not been fully elucidated. Scientific research in the field of joint diseases of the spine has not yet identified sufficiently effective methods for the complete restoration of intervertebral discs. Modern methods of treatment are aimed only at eliminating the external signs of the disease. Full recovery is currently considered impossible.
Traditional drug therapy
The rheumatologist prescribes medications, depending on the general condition of the patient. The clinical picture provides the information necessary for drawing up a treatment regimen with drugs of several groups.
- Anesthetic agents.Broad-spectrum injections, ointments or drugs are prescribed.
- Anti-inflammatory drugs (NSAIDs).
- Vasodilators.Suppression of muscle tone in the lower back and legs.
- Chondroprotectors.Designed to exclude negative progression of lumbar osteochondrosis.
Physiotherapy
Physiotherapy procedures are an integral part of inpatient or outpatient treatment of lumbar osteochondrosis.
Includes the following activities:
- Electrophoresis with painkillers;
- Magnetotherapy;
- Hydrotherapy;
- Paraffin applications.
Complex medicine and physiotherapy relieve acute pain and inflammation. But they do not guarantee stopping the progression of the pathology. Only treatment 2-3 times a year and a responsible attitude of the patient will help to avoid regression and maintain the general condition in a satisfactory form.

Exercise therapy and therapeutic massage
A set of therapeutic gymnastic exercises provides normalization of blood circulation in the lower back and helps to eliminate stagnant processes. Only a physiotherapist can prescribe exercises for clinical or home use. Typically, these are all sorts of gentle tilts and rotational movements, from a lying and sitting position. Independent physical activity can not only bring no results, but cause even more displacement of the spinal discs.
Manual therapy sessions help strengthen muscle tissue, blood flow to the affected lower back, and relieve tension. The specialist first massages on a healthy part of the back, to warm up the muscles and improve blood circulation. Then it goes to the affected areas of the lower back. The manipulation zone includes the lower back, buttocks, thighs, shins and feet. The sessions take place in regular classes, at least 10 sessions in 6 months.
Surgical intervention
It is indicated in the last stage of lumbar osteochondrosis, in order to restore the motor function of the spine. Surgery remains the only option for patients with the following symptoms:
- Constant pain syndrome, which cannot be treated even with drugs containing opiates;
- Strong compression of the nerve roots and significant displacement of the discs;
- Tumors, proliferation of bone tissue;
- Complete destruction of the vertebrae, due to constant rubbing;
- Paralysis.
Modern methods offer less traumatic methods of internal intervention. For example, endoscopy. It has a favorable prognosis, a short rehabilitation period and a low rate of side effects.

Alternative treatment
Lumbar osteochondrosis responds well to treatment with medicinal herbs and folk methods. Ointments, tinctures, baths based on fees are used to relieve swelling and pain. The most effective recipes include anesthetic and anti-inflammatory herbs:
- yarrow;
- Aloe;
- Pepper mint;
- St. John's wort;
- Spruce or pine needles;
- Wise.
The content of these herbs in folk recipes is due to their medicinal effects, scientifically proven by traditional medicine. Home treatment will help keep the lower back in a stable condition and prevent exacerbation of the disease after complex treatment.
Prevention
Although lumbar osteochondrosis is an incurable disease, its negative manifestations can be minimized. In the early stages, the disease is successfully treated, it is enough to seek timely medical help. It is important to fully adhere to the established treatment regimen and follow the recommendations of the rheumatologist.



















